Reinforcing Hand Hygiene Practices in India: Necessity and Strategies
JASPI March 2026 / Volume 4 /Issue 1
Copyright: © Author(s). This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Bhattacharjee S, Thankachan JL, Reinforcing Hand Hygiene Practices in India: Necessity and Strategies. JASPI. 2026;4(1):Page No DOI: 10.62541/jaspi114
ABSTRACT
Hand hygiene (HH) is a foundational practice in preventing the transmission of infectious diseases, yet adherence to proper hand hygiene protocols remains a global challenge, especially in India. This narrative review article probes into the significance of HH Week celebrations, barriers and facilitators of Indian practices, and advocates for sustained awareness efforts. Despite progression in healthcare and hygiene practices, non-adherence to HH guidelines persists, leading to preventable infections. Through real-life examples and evidence-based strategies, this article highlights the importance of on-going education and proposes solutions to enhance compliance with HH practices.
INTRODUCTION
Hand hygiene (HH) stands as a cornerstone of infection prevention and control in all levels of healthcare setting. It has been recognised globally for its efficacy in reducing the transmission of pathogens. Despite its proven effectiveness, adherence to proper hand hygiene practices remains a persistent challenge in various settings, including healthcare facilities (primary, secondary, and tertiary care facilities), schools, and communities. If we go back in history, we often can find that the traditional customs and beliefs of health care include hand washing and cleaning before any important day to day activity. Even in our childhood, we have witnessed our mothers and grandmothers guiding us to wash our hands and face after coming from outside, wash “our “ hands before eating, etc. Over time, this healthy habit was lost in the culture, and hand hygiene was relegated to the confines of a hospital. This review will delve deeper into the existing problem, drawing upon original studies and meta-analyses that underscore the importance of hand hygiene as one of the most successful interventions in preventing infectious diseases. The review also explores the factors contributing to fluctuating infection control rates and examine whether these fluctuations are entirely man-made and preventable.
NEED OF HH, INCLUDING CHALLENGES
Numerous systematic reviews and meta-analyses point out the significant role played by HH practices in resource constrained settings. It reduces the pathogen load and the incidence of infections like acute respiratory tract infections (ARI). However, the test on influenza and Covid 19 become inconclusive. 1,2,3
Despite numerous evidence supporting the importance of hand hygiene, challenges persist in achieving and sustaining high levels of compliance. Fluctuating infection control rates underscore the complex interplay of various factors contributing to the transmission of infectious agents. While some fluctuations may be attributed to natural variations in microbial activity and seasonal trends, many are directly linked to human behaviour and healthcare practices.
In institutions like schools, fluctuation happens due to several reasons. The factors to be pointed out are non-availability of soap and water, cost of soap and irregular water supply are the evident physical factors that create barrier to HH practise. Further lack of internal motivation to develop HH as a habit and time prioritisation over other activities are the other reasons.
In domestic settings, lack of perceived health risk and automatic motivation curtail the reflective habit of developing HH practises. Prioritising the time devoted for hand washing to other domestic responsibilities limits parents to cultivate the habit of handwashing before and after certain activities like toileting and having food.5
Despite significant efforts put for infection prevention and control, the persistence of HAIs underscores the need for continuous vigilance and improvement. Hand Hygiene Week celebrations serve as a timely reminder of the importance of hand hygiene practices in mitigating the spread of infectious diseases. India started observing hand hygiene awareness on the Global Handwashing Day promoted by WHO and UNICEF in 2008. Later, understanding its significant role in community health, Japan International Cooperation Agency (JICA)-India launched an initiative Achchi Adhat in 2021 to spread hand hygiene awareness in the community. This annual program aims to educate the community by organizing street rally, school campaigns, media advertisements and distributing sanitation items. India also launches events like National Hand Hygiene Awareness Week under Sustained Development Goal 3, in the first week of December 2025. The day is observed to educate the practise of hand hygiene among youth and general population.
SIGNIFICANCE OF HAND HYGIENE WEEK
The significance of Hand Hygiene Week cannot be overstated. This annual observance reinforces the importance of hand hygiene practices among healthcare workers, patients and the general public. The initiative educate about the role of hand hygiene in reducing the transmission of pathogens and preventing infections in various settings, including healthcare facilities, schools, and households (World Health Organization, 2009) 6. Even with the annual observance of Hand Hygiene Week and ongoing educational efforts, studies indicate a persistent gap between knowledge and practice7. While many individuals may be aware of the importance of handwashing, adherence to the recommended practices remains suboptimal in various settings. This discrepancy highlights the need for sustained educational campaigns that should go beyond the specific days and weeks designated for awareness.
Sustained educational campaigns can take various forms, including interactive workshops, distribution of informational materials, public service announcements, and social media campaigns. These initiatives should be tailored to different target audiences, taking into account the factors that may influence hand hygiene behaviours (Boyce & Pittet, 2002) 3. Also, ongoing reinforcement of key messages throughout the year is essential to instil lasting behavioural changes.
In addition to education, improving access to hand hygiene facilities is important for promoting adherence to the recommended practices. Healthcare facilities, schools, workplaces, and public spaces should ensure the availability of handwashing stations with soap and water or alcohol-based hand sanitisers. Furthermore, regular maintenance and replenishment of supplies are necessary to facilitate consistent hand hygiene practices.
FACTORS THAT CHALLENGE IN HH PRACTICES
As stated earlier, the fluctuations in infection control rate are partly due to natural phenomena, preventable manmade reasons are also contributing to the transmission of diseases. An understanding that inadequate hand hygiene practices, along with suboptimal infection prevention measures, contribute to the persistence of HAIs and community-acquired infections is the first step towards the change.
Busy work environments, inadequate access to hand hygiene facilities, lack of awareness, and misconceptions about hand hygiene efficacy are some other reasons to mention 8. Additionally, behavioural factors, such as forgetfulness and complacency, further hinder compliance with recommended hand hygiene practices 9.
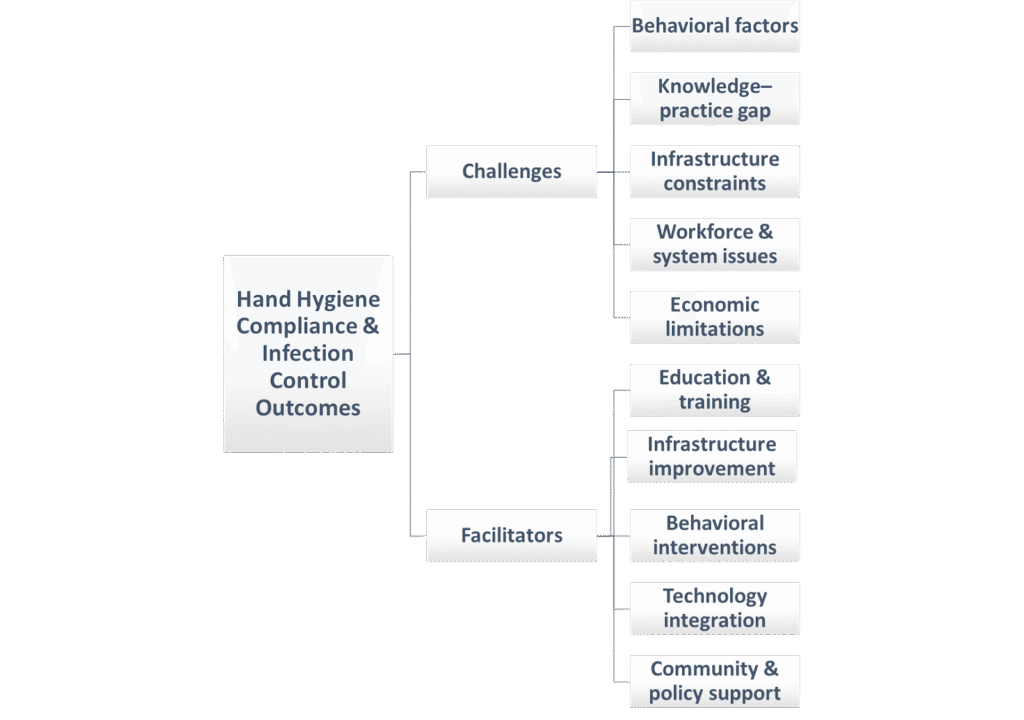
Addressing these challenges requires a multifaceted approach that encompasses education, infrastructure improvements, behavioural interventions, and robust infection control protocols.
Behavioural interventions, among the mentioned ones, are the most difficult and have limited success stories. But here lies the significance of repeated reinforcements for behavioural changes. Few instances worth mentioning are. Kourbeti I et al, in their article states that surgeons are historically claimed to be less engaging and hence they are kept aside of the routine infection prevention and control activities. One of the most significant contributors to hospital-acquired infection (HAI) cases is surgical site infection. Thus it is more important to reinforce hand hygiene practices repeatedly amongst surgeons 5.
To tackle these challenges, a multifaceted approach is necessary. Firstly, education plays a pivotal role in addressing misconceptions and raising awareness about the importance of hand hygiene. Educational campaigns should be tailored to different target audiences and delivered through various channels, including workshops, posters, and online resources 10.
Secondly, infrastructure improvements are essential to ensure adequate access to hand hygiene facilities. This includes installing hand washing stations in convenient locations, ensuring a stable supply of soap and water, and providing alcohol-based hand sanitizers in areas where hand washing facilities are not feasible 11.
Thirdly, behavioural interventions are crucial in promoting sustained adherence to hand hygiene practices. These may include implementing reminders, such as visual cues or alarms, to prompt hand hygiene actions at key times. Peer-to-peer accountability systems and feedback mechanisms can also encourage individuals to maintain hand hygiene habits 9,12.
Thus, with a multifaceted approach addressing these barriers comprehensively, healthcare facilities, schools, and other settings can promote a culture of hand hygiene and reduce the transmission of infectious diseases.
FACILITATORS TO HH PRACTICES IN INDIAN CONTEXT
Taking reference from the quality improvement practises done in a tertiary care hospital (16), the facilitators to HH practises in health care settings are
Regular supply of consumables with proper arrangement of environment to practise handwashing
Education and proper training to the staff personnel, with small group discussions, This cultivates the habit of inclusivity in the team, which develops a positive impact in the habit of handwashing. Encouraging peer group learning will also improve the motivation to do the practise in an accountable manner. Increasing awareness about the good and bad practises using the surveillance footage, followed by feedback further improves the adherence to hand hygiene practises
The study utilises the help of a proprietary product in educating the HH practices but gives a mixed impact on improving the adherence to the practice against expectations. Logistics, technical and economic reasons limit how to reap benefits through this method.
As children can learn and adapt easily, introducing an habit into them is easy. Thus, schools play an important role in inducing a behaviour change. Various activities that can be organized in schools are
forming health clubs
playing interactive games that educate children how effective handwashing keeps them safe from germs and diseases
introducing the concept of ‘health champion’
observing hand hygiene days
conducting debates, small group discussion, skits to increase awareness
providing adequate water facilities and consumables regularly
advertisements using sportsperson which increases the acceptability among children as they may be considered as role models.
A success story that can be shared is the’ WASH ‘,an initiative of several NGOs, WHO & UNICEF introduced in schools in 2014. Statistics show that the incidence of diarrheal disorders reduced by 34% and respiratory infections by 16% through this initiative. They implemented several programmes like supplying consumables, drinking water facilities, building toilets, education and training programmes, organizing interactive games etc.
The next strata for spreading awareness is at the community level. This can be done by different strategies.
organizing street plays, comedy skits
campaigns that facilitate education and proper training to HH practices have to be conducted.
objective feedback by tying with technology may help in motivational change
local government bodies should take the responsibility of providing the needed consumables and logistic support in their respective areas for strengthening of the initiative.
Combining all the facilitators of HH practices for improving the adherence nationally and globally are as follows:
Education and Training: Comprehensive hand hygiene education programs tailored to different target audiences, including healthcare professionals, patients, and caregivers, are essential. These programs should emphasise the rationale behind hand hygiene, proper techniques, and the consequences of non-adherence. The study by Gould (2017) demonstrated the effectiveness of targeted education interventions in improving nurses’ hand decontamination practices 7.
Infrastructure Improvement: Ensuring easy access to hand hygiene facilities, including handwashing stations and alcohol-based hand rubs, is another significant step. Facilities should be strategically located and well-stocked to encourage regular hand hygiene practices. According to the World Health Organisation (WHO, 2009), adequate infrastructure promotes hand hygiene compliance in healthcare settings 6.
Behavioural Interventions: Implementing behavioural nudges, such as visual reminders and social norms messaging, can positively influence hand hygiene behaviour. Peer-to-peer encouragement and feedback mechanisms promote accountability and sustain motivation. The study by Boyce and Pittet (2002) highlighted the effectiveness of social norms messaging in improving hand hygiene compliance among healthcare workers 1.
Technology Integration: integrating with the technology, such as electronic monitoring systems and smartphone applications, can provide real-time feedback on hand hygiene compliance. This facilitates continuous improvement efforts. Electronic monitoring systems have been shown to increase hand hygiene adherence rates in healthcare facilities 1. Smartphone applications that offer educational resources and reminders can empower individuals to adopt and maintain proper hand hygiene practices. The following are the two real life examples conducted in different settings to understand how technological intervention improves the habit of hand washing
Gaming technology by Sure Wash
Sure Wash is a computer-based training tool that teaches handwashing using a fun, game-like system. It shows each step of proper hand hygiene and gives instant feedback. In one hospital study, using Sure Wash helped staff improve their handwashing technique and this increased overall hand hygiene compliance from 42% to 84%. Staff enjoyed using it and repeated the training until they got a perfect score 13.
Immersive Technology like Virtual Reality (VR)
VR creates a digital environment where learners can practice hand hygiene. In a review of 11 studies, most found VR helpful for teaching hand hygiene. It made learning more engaging and improved technique, motivation, and confidence. Some VR programs even showed invisible germs to help learners understand the importance of proper hand washing 14.
Both tools make hand hygiene training more interactive and memorable. They support traditional education by offering personal feedback and hands-on practice, which helps in building lasting habits.
CONCLUSIONS
Hand Hygiene Week celebrations raise awareness and foster a culture of hand hygiene. But sustained efforts are necessary to address the persistent challenges associated with non-adherence. By implementing evidence-based strategies, including education, infrastructure improvements, behavioural interventions, and technology integration, we can enhance hand hygiene adherence and mitigate the risk of infections in various settings.
ACKNOWLEDGEMENT:
None
CONFLICT OF INTEREST STATEMENT:
Authors declare no conflict of interest.
SOURCE OF FUNDING:
None
DECLARATION FOR THE USE OF GENERATIVE ARTIFICIAL INTELLIGENCE (AI) IN SCIENTIFIC WRITING: No AI tool has been used for writing the manuscript.
AUTHORS’ CONTRIBUTIONS:
SB: Conceptualization; Analysis; Supervision Writing the draft, Validation, Review & editing
JLT: Data curation; Methodology; Resources, Writing the draft, Review & editing
REFERENCES
Allegranzi, B., & Pittet, D. (2009). Role of hand hygiene in healthcare-associated infection prevention. Journal of Hospital Infection, 73(4), 305-315.
Ross I, Bick S, Ayieko P, et al. Effectiveness of handwashing with soap for preventing acute respiratory infections in low-income and middle-income countries: a systematic review and meta-analysis. Lancet. 2023;401(10389):1681-1690. doi:10.1016/S0140-6736(23)00021-1
Boyce, J. M., & Pittet, D. (2002). Guideline for Hand Hygiene in Health-Care Settings. Recommendations of the Healthcare Infection Control Practices Advisory Committee and the HICPAC/SHEA/APIC/IDSA Hand Hygiene Task Force. MMWR. Recommendations and reports: Morbidity and mortality weekly report. Recommendations and reports, 51(RR-16), 1–45.
Haque M, McKimm J, Sartelli M, et al. Strategies to Prevent Healthcare-Associated Infections: A Narrative Overview. Risk Manag Healthc Policy. 2020;13:1765-1780. Published 2020 Sep 28. doi:10.2147/RMHP.S269315
Caruso BA, Snyder JS, O’Brien LA, LaFon E, Files K, Shoaib DM, Prasad SK, Rogers HK, Cumming O, Esteves Mills J, Gordon B, Wolfe MK, Freeman MC. Behavioural factors influencing hand hygiene practices across domestic, institutional and public community settings: a systematic review and qualitative meta-synthesis. BMJ Glob Health. 2025 Sep 16;10(Suppl 7):e018927. doi: 10.1136/bmjgh-2025-018927. PMID: 40957683; PMCID: PMC12443170.
Kourbeti I, Kamiliou A, Samarkos M. Antibiotic Stewardship in Surgical Departments. Antibiotics (Basel). 2024;13(4):329. Published 2024 Apr 4. doi:10.3390/antibiotics13040329
World Health Organization. (2009). WHO guidelines on hand hygiene in health care: first global patient safety challenge clean care is safer care. Geneva: World Health Organization.
Gould D. Nurses’ hand decontamination practice: results of a local study. J Hosp Infect. 1994;28(1):15-30. doi:10.1016/0195-6701(94)90149-x
McLaws ML, Kwok YLA. Hand hygiene compliance rates: Fact or fiction?. Am J Infect Control. 2018;46(8):876-880. doi:10.1016/j.ajic.2018.03.030
Erasmus V, Daha TJ, Brug H, et al. Systematic review of studies on compliance with hand hygiene guidelines in hospital care. Infect Control Hosp Epidemiol. 2010;31(3):283-294. doi:10.1086/650451
Picheansathian W. A systematic review on the effectiveness of alcohol-based solutions for hand hygiene. Int J Nurs Pract. 2004;10(1):3-9. doi:10.1111/j.1440-172x.2003.00457.
Allegranzi B, Pittet D. Role of hand hygiene in healthcare-associated infection prevention. J Hosp Infect. 2009;73(4):305-315. doi:10.1016/j.jhin.2009.04.019
Stewardson AJ, Sax H, Gayet-Ageron A, et al. Enhanced performance feedback and patient participation to improve hand hygiene compliance of health-care workers in the setting of established multimodal promotion: a single-centre, cluster randomised controlled trial. Lancet Infect Dis. 2016;16(12):1345-1355. doi:10.1016/S1473-3099(16)30256-0
Higgins A, Hannan MM. Improved hand hygiene technique and compliance in healthcare workers using gaming technology. J Hosp Infect. 2013 May;84(1):32-7. doi: 10.1016/j.jhin.2013.02.004. Epub 2013 Mar 14. PMID: 23498360.
Muršec D, Turk SŠ, Rozman U, Lorber M, Fijačko N, Vrbnjak D. Immersive technology and hand hygiene: scoping review. BMC Med Educ. 2024 Nov 19;24(1):1329. doi: 10.1186/s12909-024-06320-2. PMID: 39563325; PMCID: PMC11575447.
Maria A, Sooden A, Wadhwa R, Kaur R, Gaur I, Lhamo K, Nagaratna V. Improving handwashing among parent-attendants visiting a newborn unit practising family participatory care. BMJ Open Qual. 2022 Oct;11(Suppl 1):e001811. doi: 10.1136/bmjoq-2022-001811. PMID: 36270651; PMCID: PMC9594575.
Submit a Manuscript:
Copyright © Author(s) 2026. JASPI- Journal of Antimicrobial Stewardship Practices and Infectious Diseases.

